慢加急性肝衰竭急性静脉曲张出血的危险因素及预后分析
DOI: 10.3969/j.issn.1001-5256.2022.11.018
Risk factors for acute variceal bleeding in acute-on-chronic liver failure and its influence on prognosis
-
摘要:
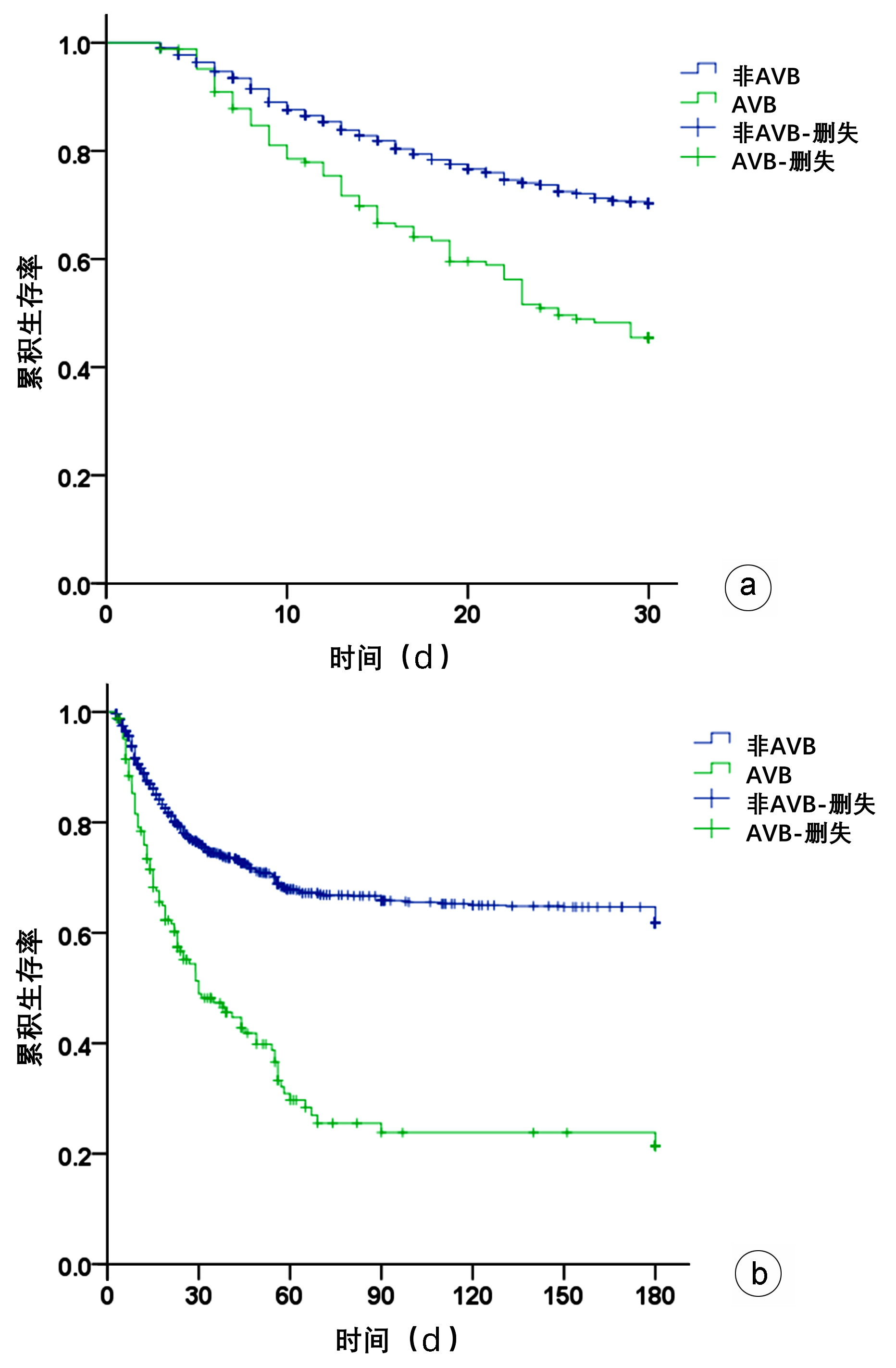
目的 探讨慢加急性肝衰竭(ACLF)急性静脉曲张出血(AVB)的危险因素及对预后的影响。 方法 对解放军总医院第五医学中心2009年—2015年收治ACLF患者1409例随访6个月,根据是否出现AVB分为AVB组(n=167)和非AVB组(n=1242)。计量资料符合正态分布两组间比较使用Student t检验;不符合正态分布资料两组间比较采用Mann-Whitney U检验。Kaplan-Meier法绘制生存曲线,对随访过程中组间病死率及进展进行Log-rank检验。采用二元Logistic回归分析AVB发生的危险因素。 结果 1409例患者发生AVB 167例,占11.85%。AVB及非AVB患者30 d存活率分别为43.42%、67.79%(χ2=33.558,P<0.001);两组患者180 d存活率分别为18.91%、53.97%(χ2=76.881,P<0.001)。Log-rank检验显示AVB与非AVB患者30 d生存率、180 d生存率差异均有统计学意义(χ2值分别为40.950、89.320,P值均<0.05)。Logistic回归分析AVB发生的危险因素,胸腔积液(OR=1.522,95%CI: 1.071 ~2.162,P=0.019)、急性肾损伤(OR=2.201,95%CI: 1.415~3.426,P<0.001)、ACLF分型(OR=2.491,95%CI: 1.489~4.168,P=0.001)、ACLF分期(OR=2.403,95%CI: 1.687~3.421,P<0.001)及尿素(OR=2.567,95%CI:1.570~4.196,P<0.001)与ACLF患者AVB的发生独立相关。 结论 AVB是影响ACLF近期生存的重要因素,胸腔积液、急性肾损伤、ACLF分型BC型、ACLF晚期以及尿素是AVB发生的独立危险因素。 Abstract:Objective To investigate the risk factors for acute variceal bleeding (AVB) in acute-on-chronic liver failure (ACLF) and its influence on prognosis. Methods A total of 1409 ACLF patients who were admitted to The Fifth Medical Center of Chinese PLA General Hospital from 2009 to 2015 were followed up for 6 months, and according to the presence or absence of AVB, they were divided into AVB group and non-AVB group. The Student's t-test was used for comparison of normally distributed continuous data between two groups, and the Mann-Whitney U test was used for comparison of non-normally distributed continuous data between two groups. The Kaplan-Meier curves were plotted and the Log-rank test was performed to analyze mortality rate and progression during follow-up, and a binary Logistic regression analysis was used to investigate the risk factors for AVB. Results Among these 1409 patients, 167 (11.85%) experienced AVB. The 30-day survival rate was 43.42% in the AVB group and 67.79% in the non-AVB group (χ2=33.558, P < 0.001), and the 180-day survival rate was 18.91% in the AVB group and 53.97% in the non-AVB group (χ2=76.881, P < 0.001). The Log-rank test showed significant differences in 30- and 180-day survival rates between the AVB group and the non-AVB group (χ2=40.950 and 89.320, both P < 0.05). The Logistic regression analysis showed that pleural effusion (odds ratio [OR]=1.522, 95% confidence interval [CI]: 1.071-2.162, P=0.019), acute kidney injury (AKI) (OR=2.201, 95%CI: 1.415-3.426, P < 0.001), ABC subtype of ACLF (OR=2.491, 95%CI: 1.489-4.168, P=0.001), ACLF stage (OR=2.403, 95%CI: 1.687-3.421, P < 0.001), and urea(OR=2.567, 95%CI: 1.570-4.196, P < 0.001)were independently associated with AVB in ACLF patients. Conclusion AVB is an important influencing factor for the short-term survival of ACLF patients, and pleural effusion, AKI, BC subtype of ACLF, advanced ACLF, and urea are independent risk factors for the onset of AVB. -
Key words:
- Acute-On-Chronic Liver Failure /
- Varicose Veins /
- Risk Factors /
- Prognosis
-
表 1 1409例ACLF基线特征
Table 1. Baseline and clinical characteristics of 1409 cases of ACLF
指标 AVB组(n=167) 非AVB组(n=1242) 统计值 P值 年龄(岁) 46.48±9.37 46.70±9.97 t=0.079 0.778 性别[例(%)] χ2=0.721 0.396 男 145(12.16) 1047(87.84) 女 22(10.14) 195(89.86) ACLF分型[例(%)] χ2=47.069 <0.001 A型 20(4.17) 460(95.83) B型 115(14.71) 667(85.29) C型 32(21.77) 115(78.23) ACLF分期[例(%)] χ2=47.902 <0.001 早期 3(8.82) 31(91.18) 中期 69(7.61) 838(92.39) 晚期 95(20.30) 373(79.70) 并发症[例(%)] 腹水 157(94.01) 1103(88.81) χ2=3.683 0.055 胸腔积液 77(46.11) 373(30.03) χ2=16.769 <0.001 肺部感染 70(41.92) 196(15.78) χ2=63.960 <0.001 SBP 80(47.90) 373(30.03) χ2=20.743 <0.001 菌血症 24(14.37) 123(9.90) χ2=3.145 0.076 肝性脑病 124(74.25) 446(35.91) χ2=88.252 <0.001 AKI 126(75.45) 497(40.02) χ2=73.500 <0.001 白蛋白(g/L) 28.89±5.73 31.20±4.26 t=6.134 0.013 TBil(μmol/L) 280.55(172.50~421.78) 284.25(194.93~388.43) Z=0.260 0.795 PTA(%) 19.01±10.93 25.72±9.77 t=67.070 <0.001 INR 2.07±0.54 2.07±0.61 t=0.011 0.917 血清钠(mmol/L) 132.47±5.87 133.29±5.89 t=2.861 0.091 胆碱酯酶(U/L) 2 583.30±1 420.97 2 770.91±1 404.29 t=2.056 0.040 纤维蛋白原(g/L) 1.68±0.90 1.74±0.96 t=0.568 0.451 血肌酐(μmol/L) 95.00(78.75~120.25) 89.00(78.00~105.00) Z=2.740 0.006 血尿素(mmol/L) 12.65(7.98~21.04) 6.70(4.60~11.30) Z=10.085 <0.001 血清铁(μmol/L) 22.16±8.63 24.61±7.79 t=13.826 <0.001 血红蛋白(g/L) 112.20(85.75~137.25) 121.70(104.00~139.00) Z=3.512 <0.001 血小板计数(×109/L) 80.32±61.09 94.01±55.35 t=8.741 0.003 MELD评分 25.82±6.69 25.40±5.36 t=0.830 0.363 MELD-Na评分 31.93±11.21 29.93±9.82 t=5.875 0.015 30 d存活率(%) 43.42(66/152) 67.79(722/1065) χ2=33.558 <0.001 180 d存活率(%) 18.91(21/111) 53.97(421/780) χ2=76.881 <0.001 表 2 Logistic回归方程中的变量
Table 2. Variables in the equation for the multilevel Logistic regression
变量 回归系数 标准误 Wald值 自由度 P值 OR 95%CI 胸腔积液 0.420 0.179 5.491 1 0.019 1.522 1.071~2.162 ACLF分型B、C型 0.913 0.263 12.089 1 0.001 2.491 1.489~4.168 ACLF分期晚期 0.877 0.180 23.644 1 <0.001 2.403 1.687~3.421 AKI 0.789 0.226 12.235 1 <0.001 2.201 1.415~3.426 尿素 0.943 0.251 14.122 1 <0.001 2.567 1.570~4.196 血小板计数 0.370 0.199 3.447 1 0.063 1.448 0.980~2.141 MELD-Na评分 -0.311 0.184 2.853 1 0.091 0.733 0.511~1.051 -
[1] SARIN SK, CHOUDHURY A, SHARMA MK, et al. Acute-on-chronic liver failure: consensus recommendations of the Asian Pacific association for the study of the liver (APASL): an update[J]. Hepatol Int, 2019, 13(4): 353-390. DOI: 10.1007/s12072-019-09946-3. [2] JOSHI D, O'GRADY J, PATEL A, et al. Cerebral oedema is rare in acute-on-chronic liver failure patients presenting with high-grade hepatic encephalopathy[J]. Liver Int, 2014, 34(3): 362-366. DOI: 10.1111/liv.12257. [3] SHIN J, YU JH, JIN YJ, et al. Acute-on-chronic liver failure as a major predictive factor for mortality in patients with variceal bleeding[J]. Clin Mol Hepatol, 2020, 26(4): 540-553. DOI: 10.3350/cmh.2020.0034. [4] TREBICKA J, GU W, IBÁÑEZ-SAMANIEGO L, et al. Rebleeding and mortality risk are increased by ACLF but reduced by pre-emptive TIPS[J]. J Hepatol, 2020, 73(5): 1082-1091. DOI: 10.1016/j.jhep.2020.04.024. [5] AL-MAHTAB M, AKBAR SM, GARG H. Influence of variceal bleeding on natural history of ACLF and management options[J]. Hepatol Int, 2016, 10(3): 436-439. DOI: 10.1007/s12072-015-9677-2. [6] Liver Failure and Artificial Liver Group, Chinese Society of Infectious Diseases, Chinese Medical Association; Severe Liver Diseases and Artificial Liver Group, Chinese Society of Hepatology, Chinese Medical Association. Diagnostic and treatment guidelines for liver failure (2018 version)[J]. J Chin Hepatol, 2019, 35(1): 38-44. DOI: 10.3969/j.issn.1001-5256.2019.01.007.中华医学会感染病学分会肝衰竭与人工肝学组, 中华医学会肝病学分会重型肝病与人工肝学组. 肝衰竭诊治指南(2018年版)[J]. 临床肝胆病杂志, 2019, 35(1): 38-44. DOI: 10.3969/j.issn.1001-5256.2019.01.007. [7] MOREAU R, JALAN R, GINES P, et al. Acute-on-chronic liver failure is a distinct syndrome that develops in patients with acute decompensation of cirrhosis[J]. Gastroenterology, 2013, 144(7): 1426-1437. e1-9. DOI: 10.1053/j.gastro.2013.02.042. [8] GARCIA-TSAO G, ABRALDES JG, BERZIGOTTI A, et al. Portal hypertensive bleeding in cirrhosis: Risk stratification, diagnosis, and management: 2016 practice guidance by the American Association for the study of liver diseases[J]. Hepatology, 2017, 65(1): 310-335. DOI: 10.1002/hep.28906. [9] HUANG Y, ZHANG W, XIANG H, et al. Treatment strategies in emergency endoscopy for acute esophageal variceal bleeding (CHESS1905): A Nationwide Cohort Study[J]. Front Med (Lausanne), 2022, 9: 872881. DOI: 10.3389/fmed.2022.872881. [10] KAMATH PS, KIM WR, Advanced Liver Disease Study Group. The model for end-stage liver disease (MELD)[J]. Hepatology, 2007, 45(3): 797-805. DOI: 10.1002/hep.21563. [11] KIM WR, BIGGINS SW, KREMERS WK, et al. Hyponatremia and mortality among patients on the liver-transplant waiting list[J]. N Engl J Med, 2008, 359(10): 1018-1026. DOI: 10.1056/NEJMoa0801209. [12] GARG H, KUMAR A, GARG V, et al. Hepatic and systemic hemodynamic derangements predict early mortality and recovery in patients with acute-on-chronic liver failure[J]. J Gastroenterol Hepatol, 2013, 28(8): 1361-1367. DOI: 10.1111/jgh.12191. [13] KAR R, KAR SS, SARIN SK. Hepatic coagulopathy-intricacies and challenges; a cross-sectional descriptive study of 110 patients from a superspecialty institute in North India with review of literature[J]. Blood Coagul Fibrinolysis, 2013, 24(2): 175-180. DOI: 10.1097/MBC.0b013e32835b2483. [14] European Association for the Study of the Liver. EASL Clinical Practice Guidelines for the management of patients with decompensated cirrhosis[J]. J Hepatol, 2018, 69(2): 406-460. DOI: 10.1016/j.jhep.2018.03.024. [15] AMITRANO L, GUARDASCIONE MA, MARTINO R, et al. Hypoxic hepatitis occurring in cirrhosis after variceal bleeding: still a lethal disease[J]. J Clin Gastroenterol, 2012, 46(7): 608-612. DOI: 10.1097/MCG.0b013e318254e9d4. [16] KUMAR A, DAS K, SHARMA P, et al. Hemodynamic studies in acute-on-chronic liver failure[J]. Dig Dis Sci, 2009, 54(4): 869-878. DOI: 10.1007/s10620-008-0421-9. [17] MEHTA G, MOOKERJEE RP, SHARMA V, et al. Systemic inflammation is associated with increased intrahepatic resistance and mortality in alcohol-related acute-on-chronic liver failure[J]. Liver Int, 2015, 35(3): 724-734. DOI: 10.1111/liv.12559. [18] TREBICKA J, GU W, IBÁÑEZ-SAMANIEGO L, et al. Rebleeding and mortality risk are increased by ACLF but reduced by pre-emptive TIPS[J]. J Hepatol, 2020, 73(5): 1082-1091. DOI: 10.1016/j.jhep.2020.04.024. [19] HEO NY. Acute-on-chronic liver failure: A predictor of poor prognosis in patients with variceal bleeding or a risk factor for variceal bleeding?[J]. Clin Mol Hepatol, 2020, 26(4): 487-488. DOI: 10.3350/cmh.2020.0209. [20] KUMAR R, KERBERT A, SHEIKH MF, et al. Determinants of mortality in patients with cirrhosis and uncontrolled variceal bleeding[J]. J Hepatol, 2021, 74(1): 66-79. DOI: 10.1016/j.jhep.2020.06.010. -



 PDF下载 ( 2154 KB)
PDF下载 ( 2154 KB)

 下载:
下载:


