炎症标志物对早期小肝癌行射频消融术预后的预测价值
DOI: 10.3969/j.issn.1001-5256.2022.04.020
Value of inflammatory biomarkers in predicting the prognosis of early small hepatocellular carcinoma after radiofrequency ablation
-
摘要:
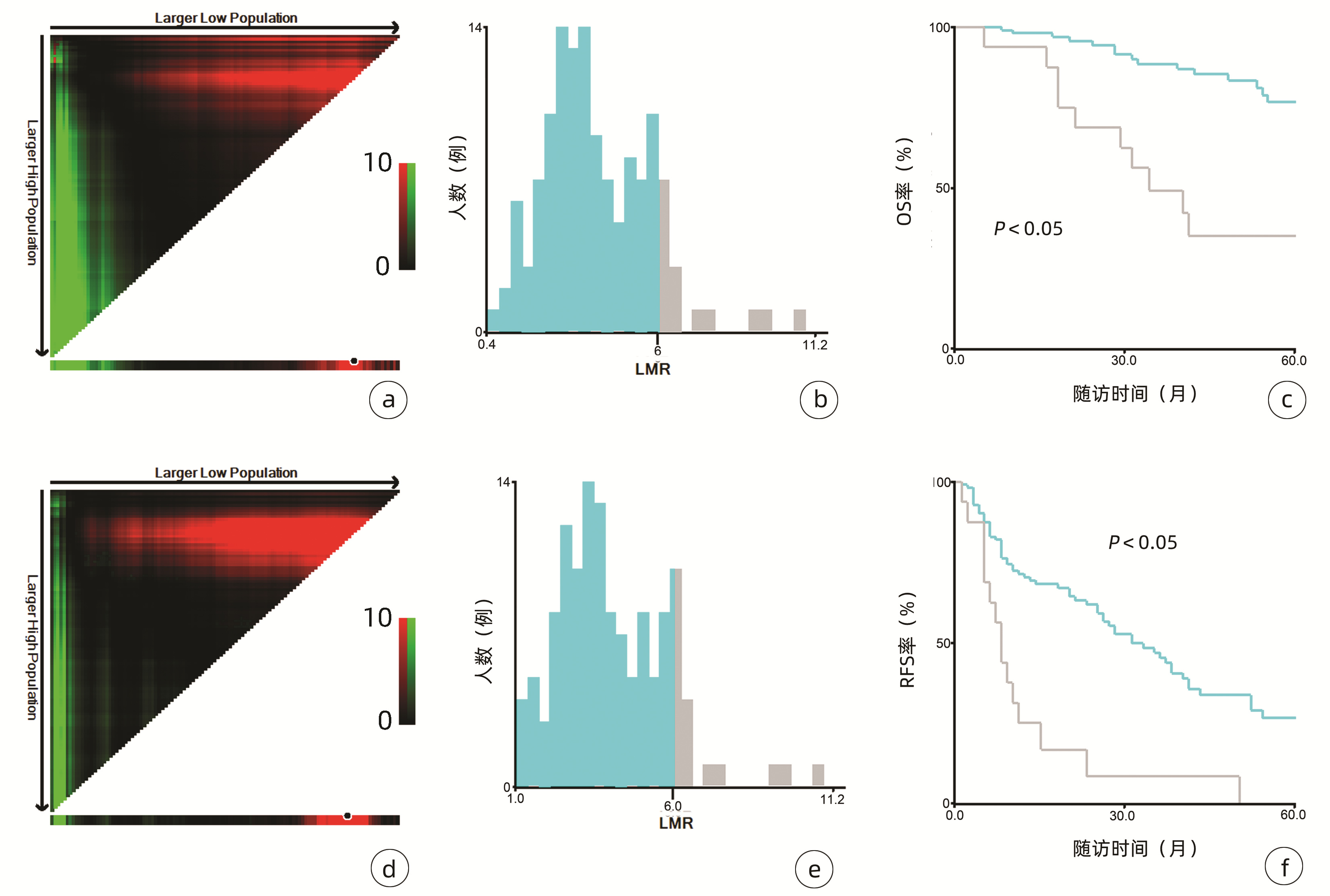
目的 探讨中性粒细胞/淋巴细胞比值(NLR)、红细胞分布宽度/淋巴细胞比值(RLR)及淋巴细胞/单核细胞比值(LMR)在早期小肝癌射频消融术后的预后价值。 方法 选取2011年9月-2020年12月在天津市第二人民医院行射频消融术的132例初诊早期肝细胞癌(HCC)患者。收集患者术前资料并随访观察复发和生存情况。运用X-tile工具以5年生存率及无复发生存率确定NLR、RLR和LMR的最佳截断值并组合成为N-R-L评分, 并据此分为N-R-L 0分组(n=92)、N-R-L 1分组(n=29)和N-R-L 2分组(n=11)。计数资料3组间比较采用χ2检验。采用Kaplan-Meier方法绘制生存曲线, 并用log-rank检验对无复发生存率及总体生存率进行组间比较。单因素分析采用log-rank检验, 并将log-rank检验分析中具有统计学意义的因素纳入多因素Cox回归分析以确定无复发生存率与总生存率的危险因素。 结果 N-R-L 0分、N-R-L 1分和N-R-L 2分组的组间Child-Pugh分级、Alb比较差异均有统计学意义(χ2值分别为10.992、5.699, P值均 < 0.05)。3组的1、3和5年总体生存率分别为100%、96.3%、90.7%, 96.6%、60.4%、41.3%和81.8%、46.8%、15.6%(χ2=38.460, P < 0.000 1);3组的1、3和5年无复发生存率分别为76.9%、52.5%、33.3%, 42.9%、13.1%、0和11.1%、0、0(χ2=35.345, P < 0.000 1)。多因素Cox回归分析显示, 肿瘤直径≥ 2 cm(HR=2.10, 95%CI: 1.28~3.43, P=0.003; HR=3.67, 95%CI: 1.58~8.52, P=0.002)、N-R-L评分1分(HR=3.14, 95%CI: 1.81~5.46, P < 0.000 1; HR=8.27, 95%CI: 3.15~21.71, P < 0.000 1)以及N-R-L评分2分(HR=2.61, 95%CI: 1.06~6.42, P=0.037; HR=14.59, 95%CI: 3.96~53.78, P < 0.000 1)是无复发生存与总生存的独立预测因素。 结论 由NLR、RLR和LMR组合而成的全身炎症反应标志物N-R-L评分是早期小肝癌射频消融术后复发和生存的独立危险因素, 可作为有用的无创生物标志物, 与肿瘤特征联合用来预测早期HCC射频消融术后的复发和生存。 -
关键词:
- 癌, 肝细胞 /
- 导管消融术 /
- 中性粒细胞/淋巴细胞比值 /
- 红细胞分布宽度/淋巴细胞比值 /
- 淋巴细胞/单核细胞比值
Abstract:Objective To investigate the value of neutrophil-to-lymphocyte ratio (NLR), red blood cell distribution width-to-lymphocyte ratio (RLR), and lymphocyte-to-monocyte ratio (LMR) in predicting the prognosis of early small hepatocellular carcinoma (HCC) after radiofrequency ablation (RFA). Methods A retrospective analysis was performed for 132 patients newly diagnosed with early HCC who underwent RFA in Tianjin Second People's Hospital from September 2011 to December 2020. Preoperative data were collected and the patients were followed up to observe recurrence and overall survival (OS). The X-tile tool was used to determine the optimal cut-off values of NLR, RLR, and LMR based on 5-year survival rate and recurrence-free survival (RFS) rate, and then the patients were divided into N-R-L 0 group with 92 patients, N-R-L 1 group with 29 patients, and N-R-L 2 group with 11 patients. The chi-square test was used for comparison of categorical data between the three groups. The Kaplan-Meier method was used to plot the survival curve, and the log-rank test was used to compare RFS and OS rates between groups. The factors with statistical significance in the log-rank test were included in the multivariate Cox regression analysis to determine the risk factors for RFS and OS rates. Results There were significant differences in Child-Pugh class and albumin between the N-R-L 0, N-R-L 1, and N-R-L 2 groups (χ22=10.992 and 5.699, both P < 0.05). The 1-, 3-, and 5-year OS rates of the three groups were 100%/96.3%/90.7%, 96.6%/60.4%/41.3%, and 81.8%/46.8%/15.6%, respectively (χ2=38.46, P < 0.000 1), and the 1-, 3-, and 5-year RFS rates of the three groups were 76.9%/52.5%/33.3%, 42.9%/13.1%/0, and 11.1%/0/0, respectively (χ2=35.345, P < 0.000 1). The multivariate Cox regression analysis showed that tumor diameter ≥ 2 cm (hazard ratio[HR]=2.10, 95% confidence interval[CI]: 1.28-3.43, P=0.003; HR=3.67, 95% CI: 1.58-8.52, P=0.002), N-R-L score of 1 point (HR=3.14, 95% CI: 1.81-5.46, P < 0.000 1; HR=8.27, 95% CI: 3.15-21.71, P < 0.000 1), and N-R-L score of 2 points (HR=2.61, 95% CI: 1.06-6.42, P=0.037; HR=14.59, 95% CI: 3.96-53.78, P < 0.000 1) were independent predictive factors for RFS and OS. Conclusion N-R-L, a systemic inflammatory response marker composed of NLR, RLR, and LMR, is an independent risk factor for recurrence and survival of early small HCC after RFA, and it can be used as a useful noninvasive biomarker in combination with tumor features to predict the recurrence and survival of early HCC after RFA. -
表 1 N-R-L评分的计分及分组方式
Table 1. Scoring and grouping of N-R-L score
变量 得分 NLR <4.1 0 ≥4.1 1 RLR <18.3 0 ≥18.3 1 LMR <6 0 ≥6 1 N-R-L NLR+RLR+LMR=0 0 NLR+RLR+LMR=1 1 NLR+RLR+LMR=2 2 注:N-R-L,NLR、RLR和LMR三项评分之和。 表 2 术前N-R-L分组患者的临床特征
Table 2. Clinical characteristics of patients in preoperative N-R-L group
临床特征 N-R-L 0分组(n=92) N-R-L 1分组(n=29) N-R-L 2分组(n=11) χ2值 P值 性别[例(%)] 0.545 0.762 男 66(71.7) 21(72.4) 9(81.8) 女 26(28.3) 8(27.6) 2(18.2) 年龄[例(%)] 0.371 0.831 <60岁 48(52.2) 17(58.6) 6(54.5) ≥ 60岁 44(47.8) 12(41.4) 5(45.5) BMI[例(%)] 2.024 0.363 <24 kg/m2 42(45.7) 9(31.0) 5(45.5) ≥24 kg/m2 50(54.3) 20(69.0) 6(54.5) Child-Pugh分级[例(%)] 10.992 0.001 A级 81(88.0) 26(89.7) 4(36.4) B级 11(12.0) 3(10.3) 7(63.6) BCLC分期[例(%)] 3.640 0.056 0期 18(19.6) 3(10.3) 0 A期 74(80.4) 26(89.7) 11(100) 肿瘤直径[例(%)] 3.876 0.144 <2 cm 53(57.6) 17(58.6) 3(27.3) ≥2 cm 39(42.4) 12(41.4) 8(72.7) HBV感染[例(%)] 1.601 0.449 否 22(23.9) 5(17.2) 4(36.4) 是 70(76.1) 24(82.8) 7(63.6) HCV感染[例(%)] 1.029 0.598 否 76(82.6) 22(75.9) 8(71.7) 是 16(17.4) 7(24.1) 3(27.3) MAFLD[例(%)] 0.367 0.832 否 56(60.9) 16(55.2) 7(63.6) 是 36(39.1) 13(44.8) 4(36.4) AFP[例(%)] 1.266 0.531 <15 ng/mL 59(64.1) 21(72.4) 6(54.5) ≥15 ng/mL 33(35.9) 8(27.6) 5(45.5) ALBI分级[例(%)] 2.845 0.092 1级 54(58.7) 16(55.2) 5(45.4) 2级 36(39.1) 13(44.8) 3(27.3) 3级 2(2.2) 0 3(27.3) TBil[例(%)] 0.904 0.636 ≤20 μmol/L 55(59.8) 16(55.2) 5(45.5) >20 μmol/L 37(40.2) 13(44.8) 6(54.5) Alb[例(%)] 5.699 0.017 ≥35 g/L 82(89.1) 23(79.3) 7(63.6) <35 g/L 10(10.9) 6(20.7) 4(36.4) ALT[例(%)] 0.109 0.741 ≤50 U/L 76(82.6) 28(96.6) 7(63.6) >50 U/L 16(17.4) 1(3.4) 4(36.4) AST[例(%)] 1.572 0.456 ≤40 U/L 71(77.2) 24(82.8) 7(63.6) >40 U/L 21(22.8) 5(17.2) 4(36.4) MELD评分[例(%)] 3.022 0.221 <9分 65(70.7) 18(62.1) 5(45.5) ≥9分 27(29.3) 11(37.9) 6(54.5) 注:ALBI分级,白蛋白-胆红素分级。 表 3 Cox回归分析RFS率的影响因素
Table 3. Results of RFS by Cox regression analysis
变量 单因素分析 多因素分析 HR(95%CI) P值 HR(95%CI) P值 性别(男/女) 1.97(1.14~3.40) 0.015 1.55(0.87~2.76) 0.136 BMI(≥24 kg/m2/<24 kg/m2) 1.22(0.77~1.92) 0.402 MAFLD(是/否) 1.03(0.65~1.61) 0.916 Child-Pugh分级(B级/A级) 2.58(1.50~4.45) 0.001 1.28(0.56~2.91) 0.564 肿瘤直径(≥2 cm/<2 cm) 2.28(1.43~3.62) 0.001 2.10(1.28~3.43) 0.003 BCLC分期(A期/0期) 2.06(0.89~4.75) 0.090 ALT(>50 U/L/≤50 U/L) 1.41(0.78~2.57) 0.260 AST(>40 U/L/≤40 U/L) 1.63(0.98~2.70) 0.058 TBil(≤20 μmol/L/>20 μmol/L) 1.69(1.07~2.65) 0.024 1.60(0.96~2.67) 0.074 Alb(<35 g/L/≥35 g/L) 2.45(1.45~4.12) 0.001 1.01(0.44~2.32) 0.974 AFP(>400 ng/mL/≤400 ng/mL) 0.81(0.33~2.01) 0.650 ALBI分级(ref: 1级) 2级 1.25(0.79~2.00) 0.341 0.92(0.49~1.70) 0.781 3级 4.15(1.61~10.70) 0.003 1.91(0.48~7.59) 0.356 MELD评分(>9分/≤9分) 1.44(0.91~2.28) 0.124 N-R-L得分(ref: 0分) 1分 3.13(1.89~5.20) <0.000 1 3.14(1.81~5.46) <0.000 1 2分 4.99(2.40~10.37) <0.000 1 2.61(1.06~6.42) 0.037 表 4 Cox回归分析OS率的影响因素
Table 4. Results of OS by Cox regression analysis
变量 单因素分析 多因素分析 HR(95%CI) P值 HR(95%CI) P值 性别(男/女) 2.17(0.88~5.33) 0.093 BMI(≥24 kg/m2/<24 kg/m2) 1.64(0.78~3.44) 0.191 MAFLD(是/否) 1.20(0.58~2.51) 0.620 Child-Pugh分级(B级/A级) 3.54(1.52~8.25) 0.003 0.99(0.28~3.52) 0.987 肿瘤直径(≥2 cm/<2 cm) 2.89(1.36~6.14) 0.006 3.67(1.58~8.52) 0.002 BCLC分期(A期/0期) 1.10(0.33~3.63) 0.880 ALT(>50 U/L/≤50 U/L) 1.21(0.46~3.17) 0.705 AST(>40 U/L/≤40 U/L) 1.30(0.58~2.94) 0.530 TBil(≤20 μmol/L/>20 μmol/L) 2.27(1.08~4.76) 0.030 1.97(0.82~4.77) 0.132 Alb(<35 g/L/≥35 g/L) 3.49(1.58~7.74) 0.002 1.36(0.36~5.09) 0.649 AFP(>400 ng/mL/≤400 ng/mL) 1.35(0.41~4.50) 0.621 ALBI分级(ref: 1级) 2级 1.67(0.78~3.56) 0.184 0.97(0.35~2.65) 0.950 3级 12.94(2.55~65.68) 0.002 2.11(0.25~17.94) 0.495 MELD评分(>9分/≤9分) 1.59(0.75~3.33) 0.224 N-R-L得分(ref: 0分) 1分 6.92(2.82~17.00) <0.000 1 8.27(3.15~21.71) <0.000 1 2分 13.50(4.68~38.91) <0.000 1 14.59(3.96~53.78) <0.000 1 -
[1] YANG JD, HAINAUT P, GORES GJ, et al. A global view of hepatocellular carcinoma: Trends, risk, prevention and management[J]. Nat Rev Gastroenterol Hepatol, 2019, 16(10): 589-604. DOI: 10.1038/s41575-019-0186-y. [2] Bureau of Medical Administration National Health Commission of the People' s Republic of China. Guidelines for diagnosis and treatment of primary liver cancer in China (2019 edition)[J]. J Clin Hepatol, 2020, 36(2): 277-292. DOI: 10.3969/j.issn.1001-5256.2020.02.007.中华人民共和国国家卫生健康委员会医政医管局. 原发性肝癌诊疗规范(2019年版)[J]. 临床肝胆病杂志, 2020, 36(2): 277-292. DOI: 10.3969/j.issn.1001-5256.2020.02.007. [3] European Association for the Study of the Liver. EASL clinical practice guidelines: Management of hepatocellular carcinoma[J]. J Hepatol, 2018, 69(1): 182-236. DOI: 10.1016/j.jhep.2018.03.019. [4] KIM GA, SHIM JH, KIM MJ, et al. Radiofrequency ablation as an alternative to hepatic resection for single small hepatocellular carcinomas[J]. Br J Surg, 2016, 103(1): 126-135. DOI: 10.1002/bjs.9960. [5] TANG JQ, HE P, SU S, et al. Short-and long-term effects of radiofrequency ablation versus minimally invasive hepatectomy in treatment of small hepatocelluar carcinoma: A Meta-analysis[J]. J Clin Hepatol, 2020, 36(2): 358-362. DOI: 10.3969/j.issn.1001-5256.2020.02.025.汤金全, 何攀, 苏松, 等. 射频消融术和微创切除术治疗小肝细胞癌短期及长期效果比较的Meta分析[J]. 临床肝胆病杂志, 2020, 36(2): 358-362. DOI: 10.3969/j.issn.1001-5256.2020.02.025. [6] LI R, CHEN HP, WANG F, et al. Application of contrast-enhanced ultrasound combined with percutaneous radiofrequency ablation in the treatment of rupture and bleeding of liver cancer[J]. Chin J Gerontol, 2020, 40(17): 3653-3656. DOI: 10.3969/j.issn.1005-9202.2020.17.021.李锐, 陈卉品, 王菲, 等. 超声造影联合经皮射频消融在肝癌破裂出血治疗中的应用[J]. 中国老年学杂志, 2020, 40(17): 3653-3656. DOI: 10.3969/j.issn.1005-9202.2020.17.021. [7] DIAKOS CI, CHARLES KA, MCMILLAN DC, et al. Cancer-related inflammation and treatment effectiveness[J]. Lancet Oncol, 2014, 15(11): e493-e503. DOI: 10.1016/S1470-2045(14)70263-3. [8] WU ML, YANG SZ, FENG XB, et al. Prognostic value of preoperative inflammatory indicators for hepatocellular carcinoma[J]. Chin J Dig Surg, 2021, 20(2): 213-219. DOI: 10.3760/cma.j.cn115610-20210125-00041.吴美龙, 杨世忠, 冯晓彬, 等. 肝细胞癌术前炎症指标的预后价值[J]. 中华消化外科杂志, 2021, 20(2): 213-219. DOI: 10.3760/cma.j.cn115610-20210125-00041. [9] HUANG J, ZHAO Y, LIAO L, et al. Evaluation of red cell distribution width to lymphocyte ratio as potential biomarker for detection of colorectal cancer[J]. Biomed Res Int, 2019, 2019: 9852782. DOI: 10.1155/2019/9852782. [10] WU J, ZHANG X, LIU H, et al. RDW, NLR and RLR in predicting liver failure and prognosis in patients with hepatitis E virus infection[J]. Clin Biochem, 2019, 63: 24-31. DOI: 10.1016/j.clinbiochem.2018.11.012. [11] CRUZ JC, WATCHMAKER JM, ALBIN MM, et al. Neutrophil/Lymphocyte ratio predicts increased risk of immediate progressive disease following chemoembolization of hepatocellular carcinoma[J]. J Vasc Interv Radiol, 2019, 30(12): 1887-1892. DOI: 10.1016/j.jvir.2019.08.001. [12] CAMP RL, DOLLED-FILHART M, RIMM DL. X-tile: A new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization[J]. Clin Cancer Res, 2004, 10(21): 7252-7259. DOI: 10.1158/1078-0432.CCR-04-0713. [13] DOYLE A, GORGEN A, MUADDI H, et al. Outcomes of radiofrequency ablation as first-line therapy for hepatocellular carcinoma less than 3cm in potentially transplantable patients[J]. J Hepatol, 2019, 70(5): 866-873. DOI: 10.1016/j.jhep.2018.12.027. [14] CHO JY, CHOI MS, LEE GS, et al. Clinical significance and predictive factors of early massive recurrence after radiofrequency ablation in patients with a single small hepatocellular carcinoma[J]. Clin Mol Hepatol, 2016, 22(4): 477-486. DOI: 10.3350/cmh.2016.0048. [15] KIM YS, LIM HK, RHIM H, et al. Ten-year outcomes of percutaneous radiofrequency ablation as first-line therapy of early hepatocellular carcinoma: Analysis of prognostic factors[J]. J Hepatol, 2013, 58(1): 89-97. DOI: 10.1016/j.jhep.2012.09.020. [16] LEE HY, RHIM H, LEE MW, et al. Early diffuse recurrence of hepatocellular carcinoma after percutaneous radiofrequency ablation: Analysis of risk factors[J]. Eur Radiol, 2013, 23(1): 190-197. DOI: 10.1007/s00330-012-2561-8. [17] GRETEN FR, GRIVENNIKOV SI. Inflammation and cancer: Triggers, mechanisms, and consequences[J]. Immunity, 2019, 51(1): 27-41. DOI: 10.1016/j.immuni.2019.06.025. [18] GRIVENNIKOV SI, GRETEN FR, KARIN M. Immunity, inflammation, and cancer[J]. Cell, 2010, 140(6): 883-899. DOI: 10.1016/j.cell.2010.01.025. [19] QUAIL DF, OLSON OC, BHARDWAJ P, et al. Obesity alters the lung myeloid cell landscape to enhance breast cancer metastasis through IL5 and GM-CSF[J]. Nat Cell Biol, 2017, 19(8): 974-987. DOI: 10.1038/ncb3578. [20] NAJAFI M, FARHOOD B, MORTEZAEE K. Contribution of regulatory T cells to cancer: A review[J]. J Cell Physiol, 2019, 234(6): 7983-7993. DOI: 10.1002/jcp.27553. [21] GOODEN MJ, de BOCK GH, LEFFERS N, et al. The prognostic influence of tumour-infiltrating lymphocytes in cancer: A systematic review with meta-analysis[J]. Br J Cancer, 2011, 105(1): 93-103. DOI: 10.1038/bjc.2011.189. [22] RASHID F, WARAICH N, BHATTI I, et al. A pre-operative elevated neutrophil: Lymphocyte ratio does not predict survival from oesophageal cancer resection[J]. World J Surg Oncol, 2010, 8: 1. DOI: 10.1186/1477-7819-8-1. [23] CHEN Y, YANG Y, ZHANG XY, et al. Nomogram based on neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio to predict recurrence in patients with hepatocellular carcinoma after radiofrequency ablation[J]. Cardiovasc Intervent Radiol, 2021, 44(10): 1551-1560. DOI: 10.1007/s00270-021-02872-8. [24] WANG C, ZHAO K, HU S, et al. A predictive model for treatment response in patients with locally advanced esophageal squamous cell carcinoma after concurrent chemoradiotherapy: Based on SUVmean and NLR[J]. BMC Cancer, 2020, 20(1): 544. DOI: 10.1186/s12885-020-07040-8. [25] POLLARD JW. Tumour-educated macrophages promote tumour progression and metastasis[J]. Nat Rev Cancer, 2004, 4(1): 71-78. DOI: 10.1038/nrc1256. [26] EVANI SJ, PRABHU RG, GNANARUBAN V, et al. Monocytes mediate metastatic breast tumor cell adhesion to endothelium under flow[J]. FASEB J, 2013, 27(8): 3017-3029. DOI: 10.1096/fj.12-224824. [27] GOYAL H, HU ZD. Prognostic value of red blood cell distribution width in hepatocellular carcinoma[J]. Ann Transl Med, 2017, 5(13): 271. DOI: 10.21037/atm.2017.06.30. [28] ZHANG X, WANG D, CHEN Z, et al. Red cell distribution width-to-lymphocyte ratio: A novel predictor for HBV-related liver cirrhosis[J]. Medicine (Baltimore), 2020, 99(23): e20638. DOI: 10.1097/MD.0000000000020600. -



 PDF下载 ( 4242 KB)
PDF下载 ( 4242 KB)


 下载:
下载: